The Microorganisms
 The tiniest life forms are bacteria, yeasts, molds, and viruses, termed “microorganisms” because of their size (micro meaning small and organism meaning living being).
The tiniest life forms are bacteria, yeasts, molds, and viruses, termed “microorganisms” because of their size (micro meaning small and organism meaning living being).
Bacteria
Bacteria are the most important microorganisms to the food processor. Most are harmless, many are highly beneficial, some indicate the probable presence of filth, disease organisms, spoilage and a few cause disease. There are thousands of species of bacteria, but all are single-celled and fall into three basic shapes: spherical, straight rods, and spiral rods. To see them, you need a microscope that magnifies about 1000-fold. All bacteria reproduce by dividing into two cells. The two cells then divide to become 4, 4 become 8, and so forth. Under ideal conditions, this doubling may occur as frequently as every 15 minutes, so that within 5 hours there will be more than a million cells from the original single cell. If there are 1000 original cells instead of a single one, there will be over 1 billion cells in 5 hours.
Some rod-shaped bacteria are capable of existing in two forms, dormant spores and active vegetative cells. Vegetative cells form spores under adverse conditions as a means of survival. Spore forms preserve the bacteria from starvation, drying, freezing, chemicals, and heat. When conditions become favorable, the spores germinate, with each spore again becoming a vegetative cell with the ability to reproduce. Among the bacteria, sporulation is not a means of reproduction since each cell forms a single spore which later germinates into a single cell again. Most sporulating bacteria that grow in the presence of air belong to the Genus Bacillus, and most that grow only in the absence of air belong to the Genus Clostridium.
Yeasts and Molds
Yeasts are oval-shaped and slightly larger than bacteria. They reproduce most often by budding. In budding each cell can produce several buds, or swellings, which break away to form new, fully formed daughter cells.
Molds as found on bread, fruit, damp paper, or other surfaces are actually composed of millions of microscopic cells joined together to form chains. The chains usually have numerous branches, called hyphae. Molds can thrive in conditions too adverse for bacteria or yeasts. They reproduce by spores that are frequently present as green or black masses on the protruding hyphae.
Yeasts and molds grow on most foods, on equipment, and building surfaces where there are small amounts of nutrient and moisture. Since bacteria grow faster, they greatly outnumber yeasts and molds in most foods. However, bacteria find conditions of low pH, moisture, or temperature and high salt or sugar unfavorable. In such environments, yeasts or molds predominate. Thus, they can be a problem in dry foods, salted fish, bread, pickles, fruits, jams, jellies, and similar commodities.
Viruses
Viruses are the smallest and simplest microorganisms. Unlike bacteria, yeasts, and molds, viruses are incapable of reproducing independently. Instead, they must first invade the cells of another living organism called the host, before they can multiply. Hence, they are parasitic. Viruses are normally specific in their selection of host cells, some infecting but one species, while others are capable of infecting closely related species. As a result, viruses which infect bacteria, called bacteriophages, cannot infect human beings or other animals. On the other hand, several animal viruses, known as zoonotis, can infect human beings.
The viruses are important to the food process in two respects:
- As a bacteriophage of lactic or other fermentative bacteria. Bacteriophage infections of starter cultures can interfere seriously with the manufacture of cheese, buttermilk, sauerkraut, pickles, wine, beer, and other desirable fermentative products.
- As disease transmitted by food to human beings. Although viruses require a live host cell and cannot multiply in foods, they can remain viable and infectious for long periods of time, even under highly adverse conditions, such as drying, freezing, and pasteurization.
Factors Affecting Growth of Microorganisms
The food processor reduces potential problems from microorganisms in several ways:
- Removing or destroying them by trimming, washing, heating, pickling, by adding chemicals, or by encouraging competition by acid- or alcohol-forming organisms.
- Minimizing contamination from equipment, people, the environment, and from unprocessed food.
- Minimizing microbial growth on equipment, by cleaning and sanitizing, and in the product itself by adjusting storage temperature, pH, and other environmental factors.
Although each factor affecting growth is considered separately in the following discussion, these factors occur simultaneously in nature. When more than one condition is somewhat adverse to microbial growth, their inhibitory effects are cumulative.
Temperature
Temperature is the most efficient means to control microbial growth. Based on their tolerance of broad temperature ranges, microorganisms are roughly classified as follows:
- Psychrophies grow only at refrigeration temperatures.
- Psychrotrophs grow well at refrigeration temperatures, but better at room temperature.
- Mesophiles grow best at or near human body temperature, but grow well at room temperature.
- Thermophiles grow only at temperatures about as hot as the human hand can endure, and usually not at all at or below body temperature.
To be more specific about these temperature limits of growth is to enter the controversy that has continued since the infancy of microbiology, for there are many species that grow in temperature ranges overlapping these. However, for food microbiology these conclusions are pertinent:
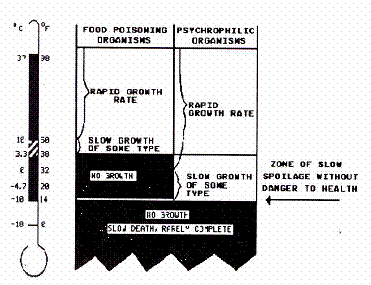
Figure 1. Low temperature limits growth of food poisoning and food spoilage organisms. (Burr and Elliot, 1960; Leistner et.al., 1975)
- Some psychrotrophic microorganisms grow very slowly in foods below freezing, but usually not below 19°F. There are a few reports of growth, usually of molds, at 14°F, but no reliable reports of growth below that temperature. This means that the standard storage temperature for frozen foods, O°F, does not permit microbial growth. However, many microorganisms survive freezing (Michener and Elliott, 1964).
- Most psychrotrophs have difficulty growing above 90°F.
- Most foodborne disease organisms are mesophiles. The food processor can feel safe in the knowledge that foods held above or below the limits in Figure 1 and rotated properly will remain safe. A good rule of thumb is to store perishable foods below 40°F or above 140°F.
- In the temperature range where both mesophilic and psychrotrophic organisms grow (about 41°F. to about 90°F), the psychrotrophs grow more rapidly, causing spoilage and at the same time frequently interfering with the growth of foodborne disease organisms (Elliott and Michener, 1965).
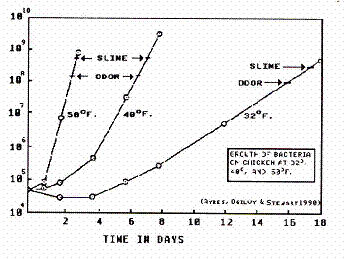
Figure 2. Growth of bacteria on chicken at three temperatures. (From data of Ayres et. al., 1950)
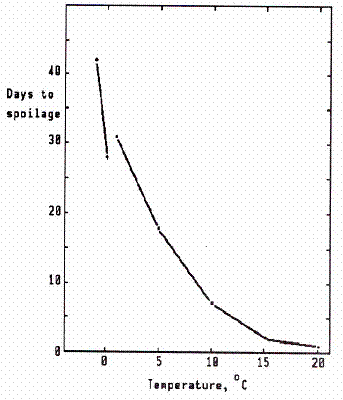
Figure 3. Effect of temperature on time for chicken meat to spoil.(From data of Lochhead and Landerkin, 1935 and Barnes and Shrimpton, 1957)
Within the growth range, the rate of growth increases rapidly as the temperature is raised (Figure 2). Conversely, microbial growth rates decrease rapidly as the temperature is lowered and, hence, food spoilage occurs much more slowly. This effect is especially marked near the freezing point. Note in Figure 3 that a drop from about 41°F to about 32°F will more than double the shelf life (time before spoilage).
Water Activity
Water activity (aw) is a term describing the availability of water to microorganisms. It is only roughly related to percent moisture. Pure water has an aw of 1.00, and the atmosphere above the water in a closed container will have an equilibrium relative humidity (ERH) of 100%. If we add an ounce of rocks to a quart of water in such a container, the ERH and the aw will not change. But if we add an ounce of salt, the ERH will fall to about 98 % and the aw to 0.98. Rocks do not dissolve in water but salt does, thereby reducing the proportion of water that can enter the atmosphere. Likewise, the amount of water available to microorganisms present in the solution is reduced. Yet the percent moisture is the same in the container with rocks as it is in the container with, salt, namely, 98%.
The GMP regulations for low-acid canned foods defined water activity as the vapor pressure of the food product divided by the vapor pressure of pure water under identical conditions of pressure and temperature. The regulations define low-acid foods as foods, other than beverages, with a finished equilibrium pH value greater than 4.6 and a water activity greater than 0.85.
| Microorganism | Minimal aw for growth | Reference |
|---|---|---|
| Salmonella | 0.945 | Christian & Scott, 1953 |
| Clostridium botulinum | 0.95 | Scott, 1957 |
| Clostridium perfringens | 0.93 | Kang, et al., 1969 |
| Staphylococcus aureus | 0.86** | Scott, 1962 |
| Vibrio parahaemolyticus | 0.94 | Beuchat, 1974 |
*These limits are the lowest reported, with all other growth conditions optimal. If other conditions are less than optimal, the minimal aw will be higher.
**Troller and Stinson (1975) have shown that minimal aw for toxin production is higher than that for growth – 0.93 in their experiments.
Most bacteria fail to grow in a food or other medium where the aw is lower than 0.94. Bacteria require a higher aw than yeasts, which in turn require a higher aw than molds. Thus, any condition that lowers the aw first inhibits bacteria, then yeasts, and finally molds (Elliott and Michener, 1965). But each species has its limits which are interrelated with other growth factors. Table 2 gives the aw limits for growth of principal foodborne disease organisms held under otherwise optimal conditions.
Certain molds and bacteria can grow on fish immersed in saturated salt solution where the aw is about 0.75. Some molds can grow in foods with aw 0.62 – 0.65 (Elliott and Michener, 1965). At these lower limits, growth is very slow. The aw of fully dried foods, such as crackers or sugar, is about 0.10 and such products are microbiologically stable because of this factor alone. The stability of intermediate moisture foods (aw 0.75 – 0.90), such as dried fruits, jams, and soft moist pet foods, depends on combinations of factors, such as low aw, low pH, pasteurization, chemical additives, and impervious packaging.
pH
pH is a term used to describe the acidity or alkalinity of a solution. At pH 7, there is an equal amount of acid (hydrogen ion: H +) and alkali (hydroxyl ion: OH-), so the solution is “neutral”. pH values below 7 are acidic, while those above 7 are alkaline. pH expresses the H + concentration logarithmically, that is, in multiples of 10. For example, at pH 5 there are 10 times as many H + as at pH 6; at pH 3 there are 100 times as many H + as at pH 5, and so on.
pH has a profound effect on the growth of microorganisms. Most bacteria grow best at about pH 7 and grow poorly or not at all below pH 4. Yeasts and molds, therefore, predominate in low pH foods where bacteria cannot compete. The lactic acid bacteria are exceptions; they can grow in high acid foods and actually produce acid to give us sour milk, pickles, fermented meats, and similar products. Some strains, called Leuconostoc contribute off-flavors to orange juice. The pH values of certain foods are given in Table 2.
| pH Value | Selected Foods |
|---|---|
| 2.3 | Lemon juice (2.3), Cranberry sauce (2.3) |
| 3.0 | Rhubarb (3.1) Applesauce (3.4), Cherries, RSP (3.4) Berries (3.0 – 3.9), Sauerkraut (3.5)Peaches (3.7), Orange juice (3.7) Apricots (3.8) |
| 4.0 | Cabbage, red (4.2), Pears (4.2) Tomatoes (4.3) |
| 4.6 | Ravioli (4.6) Pimientos (4.7) |
| 5.0 | Spaghetti in tomato sauce (4.9) Figs (5.0)Onions (5.2) Carroes (5.2) Green Beans (5.3), Beans with pork (5.3)Asparagus (5.5), Potatoes (5.5) |
| 6.0 | Lima beans (5.9), Tuna (5.9), Tamales (5.9) Codfish (6.0), Sardines (6.0), Beef (6.0) Pork (6.1), Evaporated milk (6.1) Frankfurters (6.2), Chicken (6.2) Corn (6.3) Salmon (6.4) |
| 7.0 | Crabmeat (6.8), Milk (6.8) Ripe olives (6.9) Hominy (7.0) |
The lowest pH limits for growth of foodborne disease organisms are shown in Table 3. Many of the investigators who reported these values also determined that adverse factors, such as low temperature or low water activity, increased the minimal pH for growth. But the processor can be sure that these minimal values will prevent growth of these pathogens under any and all circumstances.
| Microorganism | Growth reported at but not below | Reference |
|---|---|---|
| Staphylococcus aureus | pH 4.5 | |
| Salmonella | 4.0 | Chung and Goepfer, 1970 |
| Clostridium botulinum | ||
| Types A and B | 4.8 | National Canners Assn., 1971a |
| Type E | 5.0 | National Canners Assn., 1971a |
| Clostridium perfringens | 5.0 | |
| Vibrio parahaemolyticus | 4.8 | Beuchat, 1973 |
| Bacillus cereus | 4.9 | Kim and Goepfer, 1971 |
*Note: These limits are the lowest recorded, with all other growth conditions optimal. If other conditions are less than optimal, the pH limit will be higher.
Population
A high initial bacterial load increases the likelihood that spoilage will occur under marginal circumstances (Chung and Goepfert, 1970) (see Figures 4 and 5). This fact is of major importance to the processor of refrigerated foods, the shelf-life of which is enhanced by good sanitation. A high level of spores also increases the possibility that a few will survive to spoil heat processed products.
Oxygen
Oxygen is essential for growth of some microorganisms; these are called aerobes. Others cannot grow in its presence and are called anaerobes. Still others can grow either with or without oxygen and are called microaerophilic. Strict aerobes grow only on food surfaces and cannot grow in foods stored in cans or in other evacuated, hermetically sealed containers. Anaerobes grow only beneath the surface of foods or inside containers. Aerobic growth is faster than anaerobic. Therefore, in products where both conditions exist, such as in fresh meat, the surface growth is promptly evident, whereas subsurface growth is not.
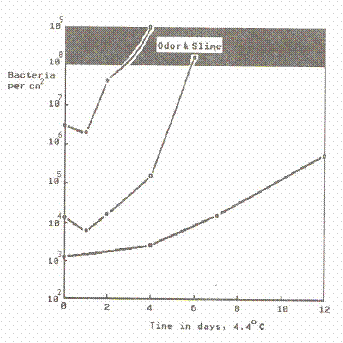
Figure 4. Effect of number of contaminating bacteria on the spoilage of chicken meat. (Ayres et. al., 1950)
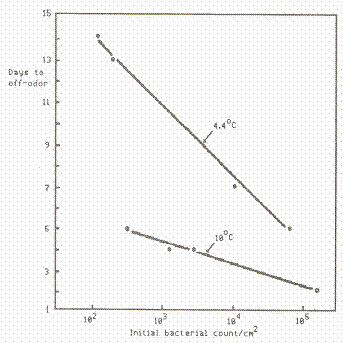
Figure 5. Effect of numbers of contaminating bacteria on the spoilage time of chicken meat. (Ayres et. al., 1950)
Lethal Effects of Temperature
Heat is the most practical and effective means to destroy microorganisms. Microbial cell reduction occurs slowly just above maximal growth temperatures. However, the rate of death increases markedly as the temperature is raised. Pasteurization, the destruction of vegetative cells of disease-producing microorganisms, consists of a temperature of 140°F for 30 minutes, or about 161°F for 16 seconds. Yeasts, molds, and the vegetative cells of spoilage bacteria also die at pasteurization temperatures. To render log-acid foods commercially sterile requires a retort capable of operating at temperatures above 212°F. Canners process certain canned foods at 240°F or 250°F for a considerable length of time, sometimes an hour or more depending upon the product and can size. Commercial sterility is the destruction and/or inhibition of the organisms of public health significance as well as organisms of non-health significance which could spoil the product. Microbiologists sterilize media at 250°F (121C) for 15 or 20 minutes. These examples illustrate the need for high temperatures and sufficient time to kill a population of bacteria.
In thermal destruction studies, also called thermal death time studies, the logarithm of the numbers of survivors is plotted against the length of time test cultures are subjected to a given temperature. The result is usually a straight line (Figure 6), although there are many exceptions (Humphrey and Nickerson, 1961). The slope of this line becomes steeper as the temperature is increased, indicating that less time is required to kill a population at higher temperatures. It also takes longer to kill a high population of organisms than it does to kill a low population (Table 4).
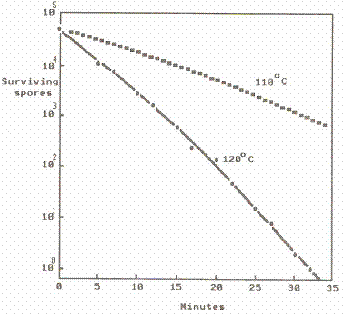
Figure 6. Reduction in numbers of bacterial spores during exposure to lethal temperatures.(Williams et. al., 1937)
The rate of thermal destruction is greater in foods with high aw than in those with low aw (Calhoun and Frazier, 1966). Microbial contaminants in dry foods, such as chocolate (Goepfert and Biggie, 1968) or dried bone meal (Riemann, 1968), are hard to destroy with heat. The recommended pasteurization process to destroy Salmonella in liquid egg albumen prior to freezing is 140°F (60C) for 3.5 minutes (USDA, 1969), whereas that for dried egg albumen is 140 (60C) to 158°F (70C) for several days (Banwart and Ayres, 1956). Riemann (1968) was able to kill Salmonella in meat and bone meal more readily at 194°F (90C) after water was added to bring the aw to 0.90.
| Microorganism | Spores (number) | Temperature °F (°C) | Destruction time (minutes) |
|---|---|---|---|
| Flat sour #26 | 45,000 | 239 (115.9) | 62 to 65 |
| 400 | 239 (115.9) | 25 to 28 | |
| Clostridium botulinum #90 | 90,000 | 221 (105.8) | 18 to 20 |
| 900 | 221 (105.8) | 12 to 14 |
Clostridium botulinum spores are highly resistant to thermal destruction at water activities between 0.2 and 0.4 (dry heat) and are much less resistant to heat at water activities above this range. This finding may be practical for high temperature-short time dry heat sterilization (National Canners Association, 1976a).
Other factors that affect the thermal destruction rate of bacteria are the presence or absence of organic matter, oil or fat, pH, strain of organisms, quality of available nutrients, and age of the culture. In general, bacteria are killed more rapidly at lower and higher pH values than in more neutral ranges. In the processing of many foods, careful control of pH is an important factor.
Chilling to temperatures below the growth range, but above freezing, stops reproduction but kills few cells except for extremely sensitive organisms, such as vegetative cells of Clostridium perfringens. Freeze kills part of a microbial population within a few hours and storage continues to be lethal at a much slower rate. The rate of population reduction varies with the nature of the food, as illustrated in Figure 7; the most rapid drop in aerobic plate count (“total count”) occurred in orange juice, which is an acid product. Bacterial spores die very slowly, if at all, during freezing and frozen storage. For example, the vegetative cells of Clostridium perfringens generally all die, but the spores survive. Staphylococcus aureus and related organisms survive well, but in most cases there is wide variation of susceptibility among microorganisms, even among closely related species (Figure 8). In any case, freezing is not a dependable means to destroy microorganisms since some cells of the original population almost always survive.
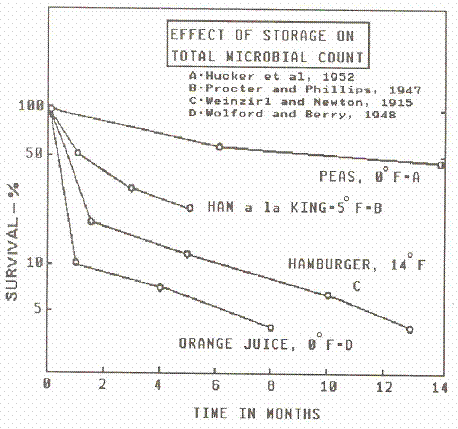
Figure 7. Effect of frozen storage on bacterial level in various foods.
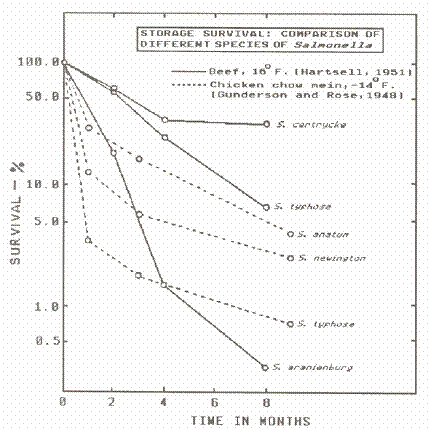
Figure 8. Survival of Salmonella in frozen storage.
The “Indicator” Organisms
The “indicator” organisms are so called because their presence in large numbers in food signifies one of three contamination possibilities: disease bacteria or filth; spoilage or low quality; or preparation under insanitary conditions.
Aerobic Plate Count
The aerobic plate count (APC) measures only that fraction of the bacterial flora that is able to grow to visible colonies under the arbitrary test conditions provided in the time period allowed. It does not measure the total bacterial population in a food sample, but is the best estimate. Altering conditions, such as composition of the agar medium or temperature of incubation, changes the spectrum of organisms that will grow. It is necessary to adhere rigidly to the standardized test conditions that have encouraged some to call the APC a “standard plate count.”
Depending on the circumstances, a high APC may indicate that a food has been grossly mishandled or that it contains a poor quality ingredient. Interpretation depends on knowing what the normal APC is for this food. An abnormal APC indicates that something is out of control. The microbiologist can frequently suggest that cause, thereby aiding the sanitarian. Some of the problems that investigation of a high APC might reveal include:
- Failure of sorting, trimming, washing, and destroying operations to remove or destroy bacteria from raw ingredients adequately.
- Inadequate heat processing.
- Insanitary equipment, particularly near the end of the process.
- The food has reached or is approaching the end of its refrigerated shelf-life.
- The food has been stored at or above room temperature for too long.
- The food is at least partly decomposed.
Coliform Bacteria
The coliform bacteria are non-spore forming rods that occur in large numbers in human and animal feces. They are normally present on raw animal products, such as meats, milk, and eggs, and also occur naturally in soil, water, and surfaces of plants. They are heat sensitive and die rapidly during blanching or pasteurizing. Large numbers of coliforms after a heat process indicate an unacceptable degree of post-heating contamination or indicate time-temperature abuse of the food sufficient to permit growth. High coliform levels warrant investigations to determine the source of contamination or temperature mishandling.
The presence of Escherichia colia, member of the coliform group, in food usually indicates direct or indirect human or animal fecal contamination. Although this may be true in a broad sense, one must not assume a quantitative relationship between the numbers of E. coli and the degree of contamination with feces. E. coli grows well outside the animal body and thrives in unclean food handling equipment.
Food Poisoning
Human illnesses caused by foodborne microorganisms are popularly referred to as food poisoning. The common use of a single classification is due primarily to similarities of symptoms of various food-related diseases (see Table 5). Apart from illness due to food allergy or food sensitivity, foodborne illness may be divided into two major classes, food infection and food intoxication. Food infection results when foods contaminated with pathogenic, invasive, food poisoning bacteria are eaten. These bacteria then proliferate in the human body and eventually cause illness. Food intoxication follows the ingestion of preformed toxic substances which accumulate during the growth of certain bacterial types in foods.
The period of time between the consumption of contaminated foods and the appearance of illness is called the incubation period. The incubation period can range anywhere from less than one hour to more than three days, depending on the causative organisms or the toxic product.
| Disease | Etiologic Agent | Incubation Period | Symptons |
|---|---|---|---|
| Botulism | Clostridium botulinum A.B.E.F toxin | Usually 1 to 2 days; range 12 hours to more than 1 week | Difficulty in swalling, double vision, difficulty in speech. Occasionally nausea, vomiting, and diarrhea in early stages. Constipation and subnormal temperature. Respiration becomes difficult, often followed by death from paralysis of muscles of respiration. |
| Staphylococcal food poisoning | Staphyloccal enterotoxin | 1 to 6 hours; average 3 hours | Nausea, vomiting, abdominal cramps, diarrhea, and acute prostration. Temperature subnormal during acute attack, may be elevated later. Rapid recovery-usually within 1 day. |
| Salmonellosis | Specific infection by Salmonella spp. | Average about 18 hours; range 7 to 72 hours | Abdominal pains, diarrhea, chills, fever, frequent vomiting, prostration. Duration of illness: 1 day to 1 week. |
| Shigellosis (bacillary dysentery) | Shigella sonnei, s. flexneri, s. dysenteriae, s. boydii | Usually 24 to 48 hours; range 7 to 48 hours | Abdominal cramps, fever, chills, diarrhea, watery stool (frequently containing blood, mucus, or pus), spasm, headache, nausea, dehydration, prostration. Duration: a few days. |
| Enteropathogenic Escherichia coli infection | Escherichia coli serotypes associated with infant and adult infections | Usually 10 to 12 hours; range 5 to 48 hours | Headache, malaise, fever, chills, diarrhea, vomiting, abdominal pain. Duration: a few days. |
| Clostridium perfringens food poisoning | Clostridium perfringens | Usually 10 to 12 hours; range 8 to 22 hours | Abdominal cramps and diarrhea, nausea, and malaise, vomiting very rare. Meat and poultry products usually involved. Rapid Recovery. |
| Bacillus cereus food poisoning | Bacillus cereus | Usually about 12 hours; range about 8 to 16 hours | Similar to Clostridium perfringens poisoning |
| Vibrio Parahaemolyticus food poisoning | Vibrio Parahaemolyticus | Usually 12 to 14 hours; range 2 to 48 hours | Abdominal pain, server watery diarrhea, usually nausea and vomiting, mild fever, chills and headache. Duration: 2 to 5 days. |
*Repeated from Prevention of Microbial and Parasitic Hazards Associated with Processed Foods, pages 6-7, with the permission of the National Academy of Sciences, Washington, DC.
Foodborne Disease Organisms
Escherichia coli
A few of the E. Coli strains found in human feces are in themselves pathogenic, causing infection and disease. These are called Enteropathogenic E. Coli or EEC. In one extensive study of the feces of food handlers (Hal and Hause, 1966), 6.4% of the workers harbored the EEC organisms as carriers.
Staphylococcus aureus
S. aureus, commonly referred to as “staph,” is normally present on the skin, the mucous membranes, and in pimples and boils of human beings and other animals. It is nearly always present in small numbers in raw meats and in foods handled extensively by human hands. The food poisoning strains generally come from human sources. Pasteurizing or cooking destroys the organism, but not its toxin. Foods contaminated by staph organisms can cause food poisoning after the organisms have been destroyed by heat.
The presence of staph in a cooked food has two levels of significance.
- Low numbers (not over a few hundred per gram) indicate the degree of contact with human skin or nasal mucous, cross-contamination from raw meat, or survivors of a larger population.
- High numbers (100,000 or more per gram) indicate that the bacteria were allowed to grow in the food, thereby creating the potential serious hazard of the presence of toxin.
Keeping foods completely free from staph contamination is often difficult or impossible. Therefore, the processor should store the food at temperatures that preclude the growth of staph (see Table 1). It is only during growth that staph forms the toxin. An epidemiological investigation to determine the source of the organism is tedious, but visual inspection of workers’ hands can be useful. The well-informed sanitarian will also seek time-temperature abuses of foods contaminated with staph.
The National Academy of Science’s National Research Council has listed the following steps to limit the incidence and level of staph in foods (NAS-NRC, 1975):
- Reduce direct and indirect exposure of foods, particularly cooked foods, to human contact as much as possible. If handling is necessary, use sanitary rubber or plastic gloves, or sanitize hands. Persons with infected cuts, abrasions, boils, or pimples should never handle cooked foods.
- Test raw materials and eliminate production lots that contain high levels of S. aureus.
- Process to destroy the microorganisms.
- Eliminate cross-contamination from raw to cooked food.
- Keep cooked foods no longer than 2 to 3 hours between 40°F and 140°F.
Control of staph growth in fermented foods, such as cheese or sausages, requires controlling a number of processing factors (see NAS-NRC, 1975). Low pH, relatively high levels of lactic bacteria, salt, and nitrite help to inhibit toxin formation.
Salmonella
Salmonella infection, or salmonellosis, is almost always caused by eating contaminated food or drink. Contamination originates from the intestinal tract of human beings or animals who harbor Salmonella organisms. Most adults can resist infection from a few cells, but become ill when ingesting millions. Infants, the aged, and the infirm are much more sensitive and can be affected by a few Salmonella cells. After recovery, the victim may remain a carrier for a period varying from a week to permanency.
Domestic animals, such as dogs, poultry, swine, horses, sheep, and cattle are carriers of these pathogens. Carriers show no outward symptoms of the disease at the time of slaughter. As long as abattoirs continue to receive Salmonella carriers for slaughter, Salmonella contamination of the finished raw meat is inevitable. Even with apparently satisfactory sanitation, slaughtering and dressing procedures may spread traces of feces from a carrier animal to subsequently slaughtered animals by way of equipment, water, and hand contact (NAS-NRC, 1969).
Salmonella is often discussed as if it were a single organism. There are actually more than 1,300 serotypes identified within the genus Salmonella. All are quite sensitive to heat, so freshly pasteurized or cooked foods are free of the organism (USDA, 1966). The principal routes of its entry into cooked foods are cross-contamination from raw foods or animals (via hands, equipment, air, water), recontamination from human carriers, or gross undercooking. Regulatory agencies are quick to institute seizures, recalls, and other legal action against products and firms shipping Salmonella-contaminated processed foods.
Dry and semi-dry fermented sausages rarely cause food borne diseases. However, recent investigations by USDA have shown that Salmonella can survive the fermentation and drying process (Smith et. al., 1975). Salmonella in natural animal casings likewise survives short periods of salting, but dies more rapidly in acidified or alkalized casings (Gabis and Silliker, 1974).
Salmonella can also grow outside the animal body when conditions are favorable. For this reason, it has appeared in a wide variety of foods and feeds, in addition to meat and poultry products. Some of these are brewers yeast, coconut meat, cochineal dye, dried or frozen eggs, noodles, custards, dried animal feeds, cottonseed flour, candy, chocolate, dried milk, fish and shellfish, cream-filled pastries, sausage casings, and watermelon. The NAS-NRC (1969-1975) has made extensive recommendations for evaluation, control, and eradication of the Salmonella problem.
Costridium botulinum
C. botulinum produces a rare but often fatal disease called botulism. It is caused by a neurotoxin produced during growth in the absence of air. Except in the case of infantile botulism the intact spores are harmless. Infants ingesting spores, usually from honey, have developed symptoms of botulism. Botulism usually occurs after a food containing the preformed toxin has been eaten, but sometimes the organism infects wounds, forming the toxin in the muscle of the victim. There are seven types of C. botulinum (A to G), of which four (A, and B associated with meats and vegetables, E, marine environment and F) cause human disease. Only once has type C been reported to cause human illness. Type G is a new incompletely studied discovery (Schmidt, 1964, USPHS, 1974).
Fortunately, the toxins, regardless of type, have very little resistance to heat and are inactivated by boiling for 10 minutes. Thus, all freshly, but adequately, cooked foods are safe (Riemann, 1973). All C. botulinum strains can form spores which exhibit varying resistance to heat. The spores of types A and B are highly resistant. Spores of type E die in a fraction of a minute at 212°F (Perkins, 1964). The canning industry, under the technical leadership of the National Food Processors Association (formerly the National Canners Association), has established times and temperatures of retorting necessary to insure the commercial sterility of low-acid canned foods (NCA, 1968, 1971b, 1976b). The NFPA also submitted to the FDA the initial petition which eventually developed in the GMP regulations for low-acid canned foods.
Botulinum spores are widely distributed in soils. Type A predominates in the western states and in New England; type B, in the eastern and southern states. Type E is usually associated with marine or fresh water environments throughout the world and is psychrotropic (Riemann, 1973). Type F has been isolated too rarely to establish its distribution pattern (Eklund et.al., 1967).
C. botulinum will not grow below pH 4.8. Therefore, botulism is a concern only in low acid foods, which are defined as foods with a finished equilibrium pH greater than 4.6. The majority of outbreaks occur from home canned vegetables, meats, fish, and over-ripe fruits (USPHS, 1974).
Canned cured meats contain salt and nitrite. The preservatives protect against the outgrowth of botulinum spores that may have survived the minimal processing, which is frequently at or below boiling (Halvorson, 1955; Ingram and Hobbs, 1954; Pivnick et. al, 1969).
There have been 34 outbreaks of type E botulism among fish products prepared in the U.S. and Canada (Lechowich, 1972). Most have been smoked or lightly salted products. The FDA isolated botulinum types B, E, and F from pasteurized meat of the blue crab (Kautter et. al., 1974). The NAS-NRC (1975) has reviewed steps to minimize the possibility of out-breaks from smoked fish and FDA has published regulations designed to control the problem (FDA, 1970).
Clostridium perfringens
C. perfringens is a spore-forming organism which, like botulinum, grows only in the absence of air. It grows best in meat or poultry dishes, stews, or gravies kept warm. Such foods meet its exacting nutritional requirements and the warm holding temperature, up to 122°F, encourages its growth. The spores themselves are harmless, but the vegetative cells, which can grow to enormous numbers in these foods, form spores in the intestinal tract of the victim. During the sporulation process, the remainder of the vegetative cell dissolves, releasing the poison that causes illness.
The vegetative cells which cause the disease are very delicate. They can be destroyed or reduced to low, safe levels by cooking or freezing. The spores are widely distributed in nature and are present in small numbers in various foods (Hall and Angelotti, 1965; Strong et. al., 1963). They occur in feces, soils, dust, water, marine sediments, raw foods, and even cooked foods.
C. perfringens poisoning is a problem specific to the food service industry. Only proper temperature control prevents the problem. A good rule of thumb is to keep ready-to-eat moist foods below 40°F or above 140°F. Time-temperature abuse is a severe health hazard. Since the spores are everywhere, epidemiologic investigation of strains to determine the source of spores is a relatively futile exercise. However, if serological tests show that the same types are present in the victim’s food and feces, a particular dish can be incriminated. Unfortunately, the biological materials (antisera) for this purpose are not yet commercially available. Therefore, the determination that large numbers of C. perfringens cells are present remains the most suitable investigative test.
Bacillus cereus
B. cereus is a spore-forming organism that grows in the presence of oxygen and is widely distributed in most raw foods. Since the spores survive boiling for several minutes, they remain viable in cooked foods in small numbers. The organism does not compete well with other bacteria in raw foods, but in moist, cooked dishes held warm (up to 122°F), it grows to millions per gram in a few hours. Under these conditions the food becomes poisonous. B. cereus grows well in a wide variety of cooked foods, such as meats, poultry, sauces, puddings, soups, rice, potatoes, and vegetables. The disease is similar to that of perfringens (see Table 5), although the mechanism of the disease is unknown. Adults have rather mild symptoms, but small children may become seriously ill. In most instances, the victims recover quickly and do not seek medical attention. Therefore, only large outbreaks are reported and become part of the statistical record.
Similar to C. perfringens, B. cereus is primarily a concern of the food service industries. The appropriate control is to keep hot foods hot (over 140°F) and cold foods cold (under 40°F). Epidemiologic investigation of strains to determine the source of the spores proves equally futile.
Vibrio parahaemolyticus
V. parahaemolyticus is a non-spore forming, slightly curved rod, closely related to the organism that causes cholera. It is widely distributed and grows in brackfish waters, estuarine sediments, raw fish, and shellfish throughout the world. It competes well with spoilage organisms at temperatures of 41°F or above. It occurs in greatest numbers in the summer when higher temperatures engender rapid growth.
V. parahaemolyticus is the principal cause of food poisoning in Japan where raw fish is regularly consumed. Elsewhere, the disease occurs less frequently because the organism dies readily during pasteurization or cooking. Nevertheless, cooked seafoods can be recontaminated from water or raw seafood. The first confirmed outbreaks in the United States occurred in 1971 and 1972 from crabmeat, shrimp, and lobster. In one Japanese outbreak, 22 people died and 250 others became ill.
The human pathogenicity of the organism is determined by culturing it on a special medium, a salt agar containing human blood. If the organism can grow and destroy blood cells on this medium, the so-called Kanagawa test, it is labeled “Kanagawa positive” and assumed capable of causing human disease. The Japanese have found that about 1% of the strains of V. parahaemolyticus from waters near their shores are Kanagawa positive (Sakazaki et. al., 1968). On the other hand, Twedt et. al. (1970) reported that up to 90% of the strains from U.S. estuarial waters are Kanagawa positive. However, the significance of the Kanagawa test is not fully understood.
To reduce the incidence of these outbreaks, the seafood industry should:
- Hold raw seafoods at or below 40°F;
- Keep cooked seafoods carefully apart from raw seafood, sea water, insanitary equipment, and unclean containers; and
- Hold cooked seafood below 40°F or above 140°F
Listeria
Before the 1980’s most problems associated with diseases caused by Listeria were related to cattle or sheep. This changed with food related outbreaks in Nova Scotia, Massachusetts, California and Texas. As a result of its widespread distribution in the environment, its ability to survive long periods of time under adverse conditions, and its ability to grow at refrigeration temperatures, Listeria is now recognized as an important food borne pathogen.
Immunocompromised humans such as pregnant women or the elderly are highly susceptible to virulent Listeria. Listeria monocytogenes is the most consistently pathogenic species causing listeriosis. In humans, ingestion of the bacteria may be marked by a flu-like illness or symptoms may be so mild that they go unnoticed. A carrier state can develop.
Following invasion of macrophages virulent strains of Listeria may then multiply, resulting in disruption of these cells and septicimia. At this time the organism has access to all parts of the body. Death is rare in healthy adults; however, the mortality rate may approximate 30% in the immunocompromised, newborn or very young.
As mentioned earlier Listeria monocytogenes is a special problem since it can survive adverse conditions. It can grow in a pH range of 5.0-9.5, in good growth medium. The organism has survived the pH 5 environment of cottage cheese and ripening Cheddar. It is salt tolerant surviving concentrations as high as 30.5% for 100 days at 39.2°F. But only 5 days if held at 98.6°F.
The key point is that refrigeration temperatures do not stop growth of Listeria. It is capable of doubling in numbers every 1.5 days at 39.2°F. Since high heat, greater than 175°F, will inactivate the Listeria organisms, post-process contamination from environmental sources then becomes a critical control point for many foods.
Yersinia enterocolitica
Even though Yersinia enterocolitica is not a frequent cause of human infection in the U.S., it is often involved in illness with very severe symptoms. Yersiniosis, infection caused by this microorganism, occurs most commonly in the form of gastroenteritis. Children are most severely affected. Symptoms of pseudo-appendicitis have resulted, in many unnecessary appendectomies. Death is rare and recovery is generally complete in 1 – 2 days. Arthritis has been identified as an infrequent but significant sequela of this infection.
Y. enterocolitica is commonly present in foods but with the exception of pork, most isolates do not cause disease. Like Listeria this organism is also one that can grow at refrigeration temperatures. It is sensitive to heat (122 F., sodium chloride (5%) and acidity (pH 4.6), and will normally be inactivated by environmental conditions that will kill salmonellae.
Campylobacter jejuni
C. jejuni was first isolated from human diarrheal stools in 1971. Since, then it has continually gained recognition as a disease causing organism in humans.
C. jejuni enteritis is primarily transferred from animal origin foods to humans in developed countries. However, fecal contamination of food and water and contact with sick people or animals predominates in developing countries.
Although milk has been most frequently identified throughout the world to be a vehicle for Campylobacter, one anticipates that future investigations will identify poultry and its products and meats (beef, pork and lamb) as major reservoirs and vehicles.
C. jejuni dies off rapidly at ambient temperature and atmosphere, and grows poorly in food.
The principles of animal science will play a significant role in the control of this ubiquitous organism. Hygienic slaughter and processing procedures will preclude cross-contamination while adequate cooling and aeration will cause a decrease in the microbial load. In addition, thorough cooking of meat and poultry products followed by proper storage should assist in maintaining food integrity and less contamination.
Mycotoxins
Mycotoxins are harmful byproducts from molds that grow on foods and feeds. They have caused severe illness and death in animals for centuries. They first came to the attention of modern scientists in 1960 when 100,000 turkey poults died in England after eating moldy peanut meal from Africa and South America. The mycotoxins involved were later shown to be aflatoxins, a group of closely related organic compounds that can cause acute disease and death. Stimulated by these first discoveries and by research in antibiotics, investigators have discovered dozens of mold strains which produce a wide variety of mycotoxins that affect animals. There are now about 60 identified toxins. Of these, only a few have been designated human food contaminants. These numbers will likely increase as mycotoxin investigations continue and identification methods are improved.
Historically, mycotoxins have been associated with human poisoning and even death. Ergot is among the first mycotoxins recognized as affecting human beings. It is produced by a mold growing on cereal grains. Ergot poisoning occurred in the Rhine Valley in the year 857 and has been reported several times since. The most recent outbreak was in 1951 in southern France. Many Russians died during World War II from eating moldy grains. The Japanese have reported human toxicity from eating moldy rice; the disease caused severe liver damage, hemorrhaging, and some fatalities (Mirocha, 1969).
Although such incidents are rare occurrences, there is evidence that low dietary levels of aflatoxins contribute to cancer of the liver in human beings. Extensive laboratory studies have also shown that even at very low dietary levels, aflatoxin can produce liver cancer in rats, mice, monkey, ducks, ferrets, and rainbow trout. Epidemiological studies in Southeast Asia and Africa have related a high incidence of human liver cancer to aflatoxin levels up to 300 parts per billion (ppb) in 20% of the food staples, and 3 to 4 ppb in 7% of the foods as eaten. In one geographical area, 95% of the corn and 80% of the peanuts contained aflatoxin at an average level of 100 ppb.
Although there is no direct evidence that aflatoxins cause human liver cancer in the United States, FDA is concerned about the effect of long-term, low-level consumption of a known, highly carcinogenic substance in our food supply. FDA established an informal defect action level tolerance of 30 ppb on peanuts and peanut products in 1965. With improved harvesting, storage, and sorting practices developed by USDA and industry, the level of aflatoxins contamination gradually declined and FDA lowered the informal action level to 20 ppb in 1969. FDA proposed in the Federal Register of December 6, 1974, a regulation establishing a tolerance of 15 ppb for total aflatoxins in shelled peanuts and peanut products used as human food. Today the limits are 0.5 ppb for milk, 20 ppb for food, and 100 ppb for feed.
Molds which form mycotoxins can be present on any food not heated in a closed container. One must assume, therefore, that they are present and capable of producing, toxin if conditions permit. But finding a toxigenic mold in a food does not imply that the food contains a mycotoxin. Conversely, the absence of visible growth of an aflatoxin producing mold does not mean toxin is absent since aflatoxins may be produced when there is little visible mold growth.
There are several ways to determine whether molds growing in an abused food will produce mycotoxins. The food can be held with its naturally contaminating molds, or inoculated with a toxigenic strain, and kept until the molds develop. The food can then be tested for the presence or absence of toxin. Such experiments have demonstrated that molds produce mycotoxins on a large variety of cereal grains and seeds, dry beans and fruits, spices, nuts, and cured meats. As do bacteria, molds have moisture, temperature, and nutritional requirements for optimal growth and toxin production. In most cases the initial mold invasion occurs in the fields before or during harvest. Mold growth continues during storage if the moisture content and storage temperatures remain high.
Aflatoxin has been found throughout the world on corn, barley, copra, cassava, spices, dry milk, tree nuts, cottonseed, peanuts, rice, wheat, and grain sorghum. In the U.S. it has been found in corn, figs, grain sorghum, cottonseed, peanuts, and certain tree nuts.
The industry has relied on electronic and visual sorting methods, as well as blowing and vacuuming, to control aflatoxin levels in walnuts arid pecans. Corn mill operators use a high intensity ultraviolet (“black”) light to detect possible aflatoxin contamination. Roasting reduces the level of aflatoxin up to 50% in some cases (Escher et. al., 1973).
The universal solution to the problem is eliminating conditions that permit mold growth, whenever it is feasible to do so, and thereby preventing the formation of mycotoxins. In some cases (corn, peanuts) mold growth and toxin production occur before harvest. Insect and bird damaged corn kernels are very susceptible; therefore, controlling these pests will help alleviate mold problems. For most susceptible foods, the critical period is immediately following harvest, during storage and initial drying when the moisture content is high enough to allow mold growth.
Spoilage
The most prevalent microbiological problem facing the food industry is simple spoilage by bacteria, yeasts, or molds that are not hazardous to health. Chilling slows spoilage; proper freezing, drying, canning, and pickling arrest it completely. Chilled foods must be transported to the consumer before spoilage microorganisms make them unfit for consumption. The problems of spoilage in the other processes arise only upon departure from established techniques. The incidence of product spoilage can be greatly reduced and shelf-life extended by taking appropriate precautions.
Refrigerated Foods
The popularity of refrigerated/chilled foods is increasing at a surprising rate. Most of these products are convenient to use and have a “close to fresh” image. Some of these products are partially cooked or processed prior to chilling. This heat reduces the microbial population but does not render it “commercially sterile.” Because of this, refrigerated foods have a limited shelf-life. That is affected by temperature and customer abuse.
Refrigerated foods have been in our stores for many years. Products such as milk, cheese, yogurt and other dairy products, cookie and biscuit doughs, eggs, salads and processed meats are commonly found in the refrigerated section or deli. The optimum storage temperature is 33°F. or as close to freezing as possible. However, most refrigerated cases are holding near 45 or even 45°F. This temperature fluctuation reduces shelf-life of the products, and can lead to a problem of public health significance.
The Refrigerated Foods and Microbiological Criteria Committee of the National Food Processors Association has published a paper on “Safety Considerations for New Generation Refrigerated Foods” in the January, 1988 issue of Dairy and Food Sanitation. Many of the points considered in this section were derived from that paper.
Several important points on preparation, handling and distribution need to be considered. First of all, always assume pathogenic organisms are present in a food product. Secondly, refrigeration temperatures may slow or prevent replication of most pathogenic microorganisms, but some will continue to multiply (psychrotrophs). Psychrotropic pathogens include Yersinia enterocolitica, Listeria monocytogenes, non-proteolytic strains of C. botulinum some strains of enterotoxigenic E. coli and Aeromonas hydrophilia. Several other food borne disease organisms capable of growth at slightly above 41°F include: Vibrio parahemolyticus; Bacillus cereus; Staphylococcus aureus and certain strains of Salmonella. Thirdly, manufacturers should expect some temperature abuse of the foods during storage and distribution; this includes handling at the consumer level.
The last two points for consideration deals with labeling. A “Keep Under Refrigeration” statement must be prominent on the product label and outside carton. In addition, a “Sell By” or “Use By” date needs to be used on these products. This will help processors control their product, but it is not a guarantee against problems. If the stock is not rotated properly, the out of date product will still get out.
A processor of refrigerated foods needs to incorporate as many treatments as possible that will help reduce the microbial population and minimize reproduction. Some of these treatments include: heat, acidification, preservatives, reduced water activity, and modified atmosphere packaging. Even though modified atmosphere is included as a potential barrier, it must be noted that reduced oxygen atmospheres may actually favor anaerobic pathogens. For many products modified atmosphere is really an aid to enhance product quality rather than safety.
One example of a product which successfully employs the multiple barrier principle is pasteurized cheese spread. The product uses a combination of reduced water activity (added salt and phosphates) and mild heat treatment to eliminate non-spore forming pathogens and inhibit growth of spore forming pathogenic microorganisms.
Any manufacturer who considers marketing a refrigerated food should have extensive shelf-life studies done by persons knowledgeable in the area of food microbiology.
Canned Foods
The shelf-life of canned foods results from the destruction of microorganisms capable of growth within the container during normal handling and storage. To attain this optimum situation, canners should:
- Follow the GMP regulations for low-acid foods.
- Reduce the spore level in the food by maintaining a sanitation program, particularly for blanchers and elsewhere where thermophilic spore formers thrive, and by monitoring ingredients for spore forming bacteria. As a general rule, food with a high spore level requires more retort time and/or temperature in the same or similar operations (Figure 6 and Table 4). A process approved by a processing authority must be filed with FDA on each low-acid and acidified food sold in the U.S. Assuming the same retort time and/or temperature, the incidence of spoilage will be higher in the canned food with a high initial spore level when all other factors are the same (Table 6).
- Follow good sanitation and good container handling techniques during the container cooling and post-cooling period. It is also important to cool heat processed containers quickly to about l00°F (38C) since thermophilic outgrowth may occur with low spore numbers if containers are stacked or cased while hot.
- Maintain good seams on cans and tight lids on glass containers by regular control and testing.
| Product | Spores per can before processing (number) | Incidence of spoilage (percent)* |
|---|---|---|
| Canned peas | 2,160 | 0 |
| 13,000 | 66 | |
| Canned corn | 900 | 16.7 |
| 38,000 | 100 |
*After incubation of processed cans at 130°F (54.4°C)
Dry Foods
Dry foods do not spoil from microbial activity once they are adequately dry. Most foods require natural or artificial drying before they become stable. Adding sugar or salt, as in candied fruits or salted fish, accomplishes the same purpose since moisture becomes unavailable for use by microorganisms. The appropriate term to express the availability of water to microorganisms is water activity (aw).
Although microorganisms cannot grow on dry foods, those that survive the drying process remain alive for prolonged periods. They quickly resume their activity upon rehydration. Under adverse conditions of storage that permit water to enter the product, molds are usually the first to grow because of their wider range of tolerance to low aw (Watson and McFarlane, 1948) and they also have less competition from other organisms.
Fermented and Pickled Foods
Fermented and pickled foods owe their stability to the microbial development of organic acids by lactic bacteria or the addition of such acids to the foods, especially in the presence of a relatively high level of salt. Spoilage can occur either during the fermentation period or upon storage of the final product. The fermentation can fail if bacteriophage attacks the starter culture, if the temperature is unsuitable, or if the amount of fermentable carbohydrate is inadequate.
To prevent spoilage during the fermentation period:
- Add lactic bacteria as a starter. Keep the starter in pure culture to help eliminate bacteriophage.
- Add fermentable carbohydrate or organic acid.
- Maintain the salt level high enough to inhibit spoilage bacteria and to permit the more salt-tolerant lactics to grow.
- Control the temperature to favor lactics.
To reduce or eliminate spoilage during storage of the pickled or fermented food:
- Add chemical preservatives, such as benzoates, sorbates, or propionates suitable to the product and acceptable to regulatory authorities.
- Pasteurize the product, if practicable, to destroy or inhibit spoilage organisms.
- Store pickles fully covered with brine to inhibit molds and impede yeast development.
